Blog
- The Brain of a Musician: Case study of Sting
- By Jason von Stietz, M.A.
- August 27, 2016
-
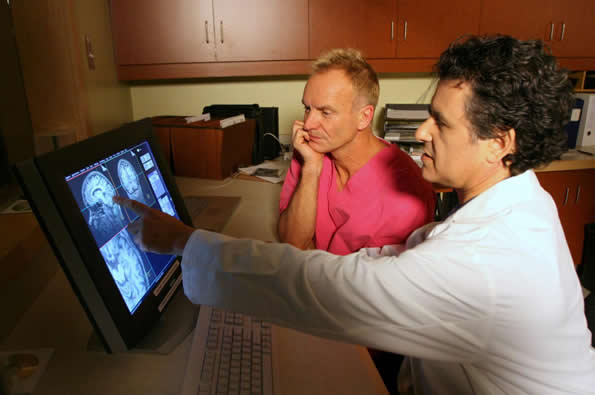
Photo Credit: Owen Egan What does musical ability look like in the brain? Researchers at McGill University were presented with a unique opportunity. In an effort to understand how a musician’s brain operates, they were able to perform brain imaging on multiple Grammy Award winning artist Sting. The study was discussed in a recent article NeuroScientistNews:
What does the 1960s Beatles hit "Girl" have in common with Astor Piazolla's evocative tango composition "Libertango?"
Probably not much, to the casual listener. But in the mind of one famously eclectic singer-songwriter, the two songs are highly similar. That's one of the surprising findings of an unusual neuroscience study based on brain scans of the musician Sting.
The paper, published in the journal Neurocase, uses recently developed imaging-analysis techniques to provide a window into the mind of a masterful musician. It also represents an approach that could offer insights into how gifted individuals find connections between seemingly disparate thoughts or sounds, in fields ranging from arts to politics or science.
"These state-of the-art techniques really allowed us to make maps of how Sting's brain organizes music," says lead author Daniel Levitin, a cognitive psychologist at McGill University. "That's important because at the heart of great musicianship is the ability to manipulate in one's mind rich representations of the desired soundscape."
Lab tour with a twist
The research stemmed from a serendipitous encounter several years ago. Sting had read Levitin's book This Is Your Brain on Music and was coming to Montreal to play a concert. His representatives contacted Levitin and asked if he might take a tour of the lab at McGill. Levitin—whose lab has hosted visits from many popular musicians over the years—readily agreed. And he added a unique twist: "I asked if he also wanted to have his brain scanned. He said 'yes'."
So it was that McGill students in the Stewart Biology Building one day found themselves sharing an elevator with the former lead singer of The Police, who has won 16 Grammy Awards, including one in 1982 for the hit single "Don't Stand So Close To Me."
Both functional and structural scans were conducted in a single session at the brain imaging unit of McGill's Montreal Neurological Institute, the hot afternoon before a Police concert. A power outage knocked the entire campus off-line for several hours, threatening to cancel the experiment. Because it takes over an hour to reboot the fMRI machine, time grew short. Sting generously agreed to skip his soundcheck in order to do the scan.
Levitin then teamed up with Scott Grafton, a leading brain-scan expert at the University of California at Santa Barbara, to use two novel techniques to analyze the scans. The techniques, known as multivoxel pattern analysis and representational dissimilarity analysis, showed which songs Sting found similar to one another and which ones are dissimilar—based not on tests or questionnaires, but on activations of brain regions.
"At the heart of these methods is the ability to test if patterns of brain activity are more alike for two similar styles of music compared to different styles. This approach has never before been considered in brain imaging experiments of music," notes Scott Grafton.
Unexpected connections
"Sting's brain scan pointed us to several connections between pieces of music that I know well but had never seen as related before," Levitin says. Piazzola's "Libertango" and the Beatles' "Girl" proved to be two of the most similar. Both are in minor keys and include similar melodic motifs, the paper reveals. Another example: Sting's own "Moon over Bourbon Street" and Booker T. and the MG's "Green Onions," both of which are in the key of F minor, have the same tempo (132 beats per minute) and a swing rhythm.
The methods introduced in this paper, Levitin says, "can be used to study all sorts of things: how athletes organize their thoughts about body movements; how writers organize their thoughts about characters; how painters think about color, form and space."
Read the original article Here
- Comments (0)
- The Myth of the Second Head Trauma Cure
- By Jason von Stietz, M.A.
-

According to cartoons and other popular media, the only cure for head trauma induced amnesia is a second head trauma. When a cartoon characters such as Fred Flintsone loses his memory following a lump on the head, it is only a second lump that brings it back. This idea seems silly to modern scientists and clinicians. However, where did this myth come from? The history of this myth was discussed in a recent article in Drexel Now:
While that worked in “The Flintstones” world and many other fictional realms, the medical community knows that like doesn’t cure like when it comes to head trauma.
However, a shockingly high level of the general public endorse the Flintstones solution, with 38–46 percent believing that a second blow to the head could cure amnesia, according to Drexel’s Mary Spiers. And, believe it or not, that belief was spurred by members of the medical community dating as far back as the early 19th century.
Spiers, PhD, associate professor in the College of Arts and Sciences’ Department of Psychology, traced the origins of the double-trauma amnesia cure belief in a paper for Neurology titled, “The Head Trauma Amnesia Cure: The Making of a Medical Myth.”
For a long time, scientists worked to figure out why the brain had two hemispheres.
“Studying the brain in the past was very challenging for several reasons,” Spiers explained. “There was no way to look into the living brain, as powerful functional imaging now allows us to do. Also, many people, including physicians, philosophers and those in the arts, speculated about the function of the brain, the soul and consciousness, so there were many competing ideas.”
At one point, scientists landed on the idea that it was a double organ, like a person’s eyes or ears, two pieces that were redundant — doing the same work.
Around the turn of the 19th century, a French scientist named Francois Xavier Bichat decided that the two hemispheres acted in synchrony. One side mirrored the other, and vice versa.
As such, he reasoned that an injury to one side of the head would throw off the other, “untouched” side.
“[Bichat] seriously proposed the notion that a second blow could restore the wits of someone who had a previous concussion,” Spiers wrote in her paper. “Bichat justified this idea by reasoning that hemispheres that are in balance with each other functioned better, while those out of balance cause perceptual and intellectual confusion.”
Bichat never cited any specific cases to back up his theory and, ironically enough, he died of a probable head injury in 1802.
“From my reading of Bichat’s work, it seems that he felt that the second trauma amnesia cure was a common occurrence and didn’t need the citation of an individual case,” Spiers said. “This was not unusual at the time, to forgo evidence like that.”
Despite backup to his claims, Bichat’s ideas continued on after his death and became known as Bichat’s Law of Symmetry. Books in the following decades cited brain asymmetry as the root of different mental health issues.
Compounding the symmetry idea was also the dominant thought that human memories could never be lost. However, Samuel Taylor Coleridge — a philosopher, not a physician — was credited with popularizing that idea.
It wasn’t until the mid-1800s that scientists began to realize that taking a hit to the head might just destroy memories completely. A second blow wasn’t likely to jump-start the brain, they realized, but create further damage.
By this time, however, enough anecdotes about curing amnesia with a second head trauma were floating around from otherwise respectable scientists that the theory invaded the general public’s consciousness. With “no hard and fast lines between scientific and popular writing,” myths like the second trauma amnesia cure circulated out of control, according to Spiers.
Even as modern scientists began to fully understand the brain, the theory still stuck with a large amount of the public, resulting in the lumps we continue to see on cartoon characters’ heads.
“One of the issues we see in the persistence of this myth is that understanding how the brain forgets, recovers and/or loses information is a complicated matter that is still being studied by brain scientists,” Spiers said. “As individuals, we may have had the experience of a ‘memory jog’ or cue that reminds us of a long-forgotten memory. Because our own experiences serve as powerful evidence to us, this reinforces the myth that all memories are forever stored in the brain and only need some sort of jolt to come back.”
But, obviously, that jolt isn’t exactly advisable.
“In the case of a traumatic brain injury, learning and memory may be temporarily or permanently impaired due to swelling and injured or destroyed neurons,” Spiers concluded. “Some memories may return as the brain recovers, but a second brain injury is never a good treatment for a first brain injury.”
Read the original Here
- Comments (0)
- Study Identifies Biomarkers for Alzheimer's Disease
- By Jason von Stietz, M.A.
- August 15, 2016
-
.jpg)
Getty Images Researchers at the University of Wisconsin Madison have identified biomarkers helpful in predicting the development of Alzheimer’s disease. The researchers analyzed the data of 175, which included brain scans, measures of cognitive abilities, and genotyping. The study was discussed in a recent article in NeuroscientistNews:
This approach – which statistically analyzes a panel of biomarkers – could help identify people most likely to benefit from drugs or other interventions to slow the progress of the disease. The study was published in the August edition of the journal Brain.
"The Alzheimer's Association estimates that if we had a prevention that merely pushed back the clinical symptoms of the disease by five years, it would almost cut in half the number of people projected to develop dementia,'' says Annie Racine, a doctoral candidate and the study's lead author. "That translates into millions of lives and billions of dollars saved."
Dr. Sterling Johnson, the study's senior author, says that while brain changes – such as the buildup of beta-amyloid plaques and tangles of another substance called tau – are markers of the disease, not everyone with these brain changes develops Alzheimer's symptoms.
"Until now, we haven't had a great way to use the biomarkers to predict who was going to develop clinical symptoms of the disease,'' Johnson says. "Although the new algorithm isn't perfect, now we can say with greater certainty who is at increased risk and more likely to decline."
The research team recruited 175 older adults at risk for Alzheimer's disease, and used statistical algorithms to categorize them into four clusters based on different patterns and profiles of pathology in their brains. Then, the researchers analyzed cognitive data from the participants to investigate whether these cluster groups differed on their cognitive abilities measured over as many as 10 years.
As it turns out, the biomarker panels were predictive of cognitive decline over time. One cluster in particular stood out. The group that had a biomarker profile consistent with Alzheimer's – abnormal levels of tau and beta-amyloid in their cerebrospinal fluid – showed the steepest decline on cognitive tests of memory and language over the 10 years of testing. About two-thirds of the 22 people sorted into this group were also positive for the APOE4 gene—the greatest known risk factor for sporadic Alzheimer's disease—compared with about one-third in the other clusters.
At the other end of the spectrum, the largest group, 76 people, were sorted into a cluster that appears to be made up of healthy aging individuals. They showed normal levels on the five biomarkers and did not decline cognitively over time.
In between, there were two clusters that weren't classified as Alzheimer's but who don't seem to be aging normally either. A group of 32 people showed signs of mixed Alzheimer's and vascular dementia. They had some of the amyloid changes in their cerebrospinal fluid, but also showed lesions in their brains' white matter, which indicate scarring from small ischemic lesions which can be thought of as minor silent strokes.
The other cluster of 45 people had signs of brain atrophy, with brain imaging showing that the hippocampus, the brain's memory center, was significantly smaller than the other groups. The authors speculate this group could have intrinsic brain vulnerability or could be affected by some other process that differentiates them from healthy aging. Both the in-between clusters showed non-specific decline on a test of global cognitive functioning, which further differentiates them from the healthy aging cluster.
The study participants came from a group of more than 1,800 people enrolled in two studies – the Wisconsin Alzheimer's Disease Research Center (WADRC) study and the Wisconsin Registry for Alzheimer's Prevention (WRAP). Both groups are enriched for people at risk for getting Alzheimer's because about ¾ of participants have a parent with the disease.
"This study shows that just having a family history doesn't mean you are going to get this disease," Johnson says. "Some of the people in our studies are on a trajectory for Alzheimer's, but more of them are aging normally, and some are on track to have a different type of brain disease." A comprehensive panel of biomarkers – such as the one evaluated in this study – could help to predict those variable paths, paving the way for early interventions to stop or slow the disease.
The authors of the study are affiliated with the WADRC, the Wisconsin Alzheimer's Institute, the Institute on Aging, the Waisman Center, and the Neuroscience and Public Policy program, all at UW-Madison; and the Geriatrics Research Education and Clinical Center at the William S. Middleton Veterans Hospital.
Read the original Here
- Comments (0)


 Subscribe to our Feed via RSS
Subscribe to our Feed via RSS