Blog
- Possible "Depression Switch" to Guide Deep Brain Stimulation
- By Jason von Stietz, M.A.
- October 10, 2015
-

Photo Credit: Getty Images Researchers at Emory University School of Medicine studied the impact of deep brain stimulation on chronic and treatment resistant depression. Findings may provide researchers with a structural “depression switch” that may guide the use of deep brain stimulation in the future. The study was discussed in a recent article in MedicalXpress:
A "depression switch" has been mapped during intraoperative deep brain stimulation of the subcallosal cingulate, according to research published online Sept. 26 in JAMA Neurology.
Ki Sueng Choi, Ph.D., from the Emory University School of Medicine in Atlanta, and colleagues characterized the structural connectivity correlates of deep brain stimulation-evoked behavior effects using probabilistic tractography in depression. Data were included for nine adults undergoing deep brain stimulation implantation surgery for chronic treatment-resistant depression.
The researchers recorded 72 active and 36 sham trials among the patients. Stereotypical behavior patterns included changes in interoceptive and in exteroceptive awareness. For all nine patients, the best response was a combination of exteroceptive and interoceptive changes at a single left contact. The best response contacts had a pattern of connections to the bilateral ventromedial frontal cortex (via forceps minor and left uncinate fasciculus) and to the cingulate cortex (via left cingulum bundle); only cingulate involvement was seen in behaviorally salient but non-best contacts.
"This analysis of transient behavior changes during intraoperative deep brain stimulation of the subcallosal cingulate and the subsequent identification of unique connectivity patterns may provide a biomarker of a rapid-onset depression switch to guide surgical implantation and to refine and optimize algorithms for the selection of contacts in long-term stimulation for treatment-resistant depression," the authors write.
Two authors disclosed financial ties to medical device companies, including Medtronic and St. Jude Medical, both of which develop products related to the research in this article. St. Jude Medical also donated the study device.
Read the original article Here
- Comments (0)
- Study Links Optimism, Anxiety, and Orbitifrontal Cortex Size
- By Jason von Stietz, M.A.
- October 3, 2015
-

Photo Credit: Getty Images Can optimism be traced to a structure in the brain? Researchers at the University of Illinois have linked optimism, anxiety, and the orbitofrontal cortex (OFC). Their study found that those with a larger OFC tend to report more optimism and less anxiety. The study was discussed in a recent article in MedicalXpress:
The new analysis, reported in the journal Social, Cognitive and Affective Neuroscience, offers the first evidence that optimism plays a mediating role in the relationship between the size of the OFC and anxiety.
Anxiety disorders afflict roughly 44 million people in the U.S. These disorders disrupt lives and cost an estimated $42 billion to $47 billion annually, scientists report.
The orbitofrontal cortex, a brain region located just behind the eyes, is known to play a role in anxiety. The OFC integrates intellectual and emotional information and is essential to behavioral regulation. Previous studies have found links between the size of a person's OFC and his or her susceptibility to anxiety. For example, in a well-known study of young adults whose brains were imaged before and after the colossal 2011 earthquake and tsunami in Japan, researchers discovered that the OFC actually shrank in some study subjects within four months of the disaster. Those with more OFC shrinkage were likely to also be diagnosed with post-traumatic stress disorder, the researchers found.
Other studies have shown that more optimistic people tend to be less anxious, and that optimistic thoughts increase OFC activity.
The team on the new study hypothesized that a larger OFC might act as a buffer against anxiety in part by boosting optimism.
Most studies of anxiety focus on those who have been diagnosed with anxiety disorders, said University of Illinois researcher Sanda Dolcos, who led the research with graduate student Yifan Hu and psychology professor Florin Dolcos. "We wanted to go in the opposite direction," she said. "If there can be shrinkage of the orbitofrontal cortex and that shrinkage is associated with anxiety disorders, what does it mean in healthy populations that have larger OFCs? Could that have a protective role?"
The researchers also wanted to know whether optimism was part of the mechanism linking larger OFC brain volumes to lesser anxiety.
The team collected MRIs of 61 healthy young adults and analyzed the structure of a number of regions in their brains, including the OFC. The researchers calculated the volume of gray matter in each brain region relative to the overall volume of the brain. The study subjects also completed tests that assessed their optimism and anxiety, depression symptoms, and positive (enthusiastic, interested) and negative (irritable, upset) affect.
A statistical analysis and modeling revealed that a thicker orbitofrontal cortex on the left side of the brain corresponded to higher optimism and less anxiety. The model also suggested that optimism played a mediating role in reducing anxiety in those with larger OFCs. Further analyses ruled out the role of other positive traits in reducing anxiety, and no other brain structures appeared to be involved in reducing anxiety by boosting optimism.
"You can say, 'OK, there is a relationship between the orbitofrontal cortex and anxiety. What do I do to reduce anxiety?'" Sanda Dolcos said. "And our model is saying, this is working partially through optimism. So optimism is one of the factors that can be targeted."
"Optimism has been investigated in social psychology for years. But somehow only recently did we start to look at functional and structural associations of this trait in the brain," Hu said. "We wanted to know: If we are consistently optimistic about life, would that leave a mark in the brain?"
Florin Dolcos said future studies should test whether optimism can be increased and anxiety reduced by training people in tasks that engage the orbitofrontal cortex, or by finding ways to boost optimism directly.
"If you can train people's responses, the theory is that over longer periods, their ability to control their responses on a moment-by-moment basis will eventually be embedded in their brain structure," he said.
Read the full article Here
- Comments (0)
- Football Player Enhances Performance with Neurofeedback
- By Jason von Stietz, M.A.
- September 27, 2015
-

Photo Credit: Getty Images Washington Redskins quarterback Kirk Cousins has revitalized his career through not only hard work and a change in outlook but also through the use of neurofeeback training. Cousins first utilized neurofeedback during his senior year at Michigan state and again this February as he revamped his approach to his craft. Cousins new approach and experience with neurofeedback was recently discussed in an article in the Washington Post:
From the moment the Washington Redskins drafted him three rounds behindRobert Griffin III in 2012, Michigan State’s Kirk Cousins was reduced to a fallback plan. He was the football equivalent of a college applicant’s “safety school” or the friend who fills in as a prom date after true love fails.
Handed the chance to prove he could be more, Cousins stumbled last season, undercutting his 10 touchdowns passes with nine grievously timed interceptions while filling in for the injured Griffin. Even Cousins’s body language conceded defeat as he trudged off the field in Week 7, head bowed, following that ninth errant throw. He was replaced by Colt McCoy and relegated to scout-team duty the rest of the year.
Less than 11 months later, Redskins Coach Jay Gruden stepped to a microphone at Redskins Park and uttered the improbable.
“It’s Kirk’s team,” Gruden said, announcing Aug. 31 that Cousins would be the team’s starting quarterback in 2015.
Cousins hadn’t played a down in a regular season game since his benching last fall. But after a solid showing in training camp, followed by a productive preseason performance, he convinced Gruden that he represents the best hope of turning around a team with back-to-back losing seasons.
But is Cousins simply the Redskins’ best available fallback plan? Or has Cousins, at 27, learned to leverage his strengths and minimize his shortcomings after a three-year NFL apprenticeship of waiting, watching and too often short-circuiting in the limited opportunities he has had?
At first glance, little has changed about the 6-foot-3, 202-pound Cousins entering Year 4, apart from a beard that hints at a new steeliness.
Washington Redskins quarterback Kirk Cousins practiced at Estero High School near Fort Myers this winter with members of the school's varsity football team.
The overhaul of consequence, Gruden believes, is Cousins’s mental game.
His offseason work included copious film study and tutoring from a private throwing coach, as is common among NFL quarterbacks. But it included unlikely assists from a few dozen high school receivers who ran pass patterns and caught balls during Cousins’s winter vacations in Georgia and Florida and a Michigan-based company called Neurocore that Cousins said “retrained” his brain to operate in a “sweet spot” best suited to peak athletic performance.
“It’s kind of an abstract thing, but I call it brain performance,” Cousins said of his training with Neurocore Brain Performance Center, which he intensified after getting benched last fall. “I see it as the next frontier because you look at weightlifting in the 1950s and ’60s, not every football player was lifting weights; they weren’t sure about the benefit it would give you. Now everybody has a strength coach; everybody lifts weights. And I see brain training kind of being that next thing. I just want to maximize what I’ve got.”
The son of a minister and a man of deep faith, Cousins conceded that dark times followed his benching in October. The NFL career he had labored for seemed at hand after he took over for Griffin and led five touchdown drives in a 41-10 rout of Jacksonville in Week 2.
The next week, he threw for 427 yards at Philadelphia. The Redskins lost, and Cousins’s play deteriorated from there. After a 45-14 loss to the New York Giants in which he threw four second-half interceptions, Giants defenders said Cousins was telegraphing his throws.
“Anytime you have a job to do and you feel like you didn’t get the job done, it’s going to eat at you if you care about it,” Cousins said this week when asked about his mind-set after his Oct. 19 benching. “For me, I deeply care about it, and so it was eating at me.”
The turning point came, Cousins said, when he quit berating himself.
“What do I do now?” he asked himself. “What can I do to get better and deliberately practice, whatever that is.”
Once Griffin was back in the starting job and McCoy named the No. 2 quarterback, Cousins was ruled inactive. With no need to prepare for the upcoming opponent, he devoted his film-study to poring over footage of the NFL’s better quarterbacks and taking a hard look at his own footage.
When February came, Cousins and his wife, Julie, traveled to Florida’s Gulf Coast for vacation. But he wanted to keep working on his game, so he phoned a local high school near Fort Myers. He introduced himself, explained that he had his cleats and a couple footballs with him and asked whether the football coach could round up some receivers to throw to and let them use the Estero High field for a workout.
Cousins’s throwing coach, former NFL quarterback Jeff Christensen, flew in from Chicago to supervise. And for three days, Cousins threw to teenagers.
“He was dead on every time,” Estero Coach Jeff Hanlon recalled in a phone interview. “There was never a bad throw. Sometimes there was something he wasn’t happy with — maybe the height on the ball — and he wanted to adjust it. . . .
“And with every throw, he said something encouraging to the kids. Even if it was a dropped pass, he’d say, ‘Hey, great route!’ Whatever it was, he found something positive in every single rep that gave that motivation and encouragement to the kids.”
While in Florida, Cousins, joined by Redskins running back Alfred Morris, also worked with Gruden’s brother, Super Bowl champion coach turned ESPN analyst Jon Gruden, who mentors young quarterbacks in the offseason.
And while in Atlanta visiting his wife’s family, he also tracked down high school receivers to throw to.
Also in February, he ramped up his training with Neurocore, which he had begun his senior season at Michigan State.
Neurocore was founded roughly 10 years ago to help children with attention-deficit disorders through “neurofeedback” rather than medication and expanded to applications for people with sleep and anxiety disorders as well as elite athletes. Its brain-training system starts with electroencephalograms to measure the electrical activity in the brain. If the data suggests the brain is running faster or slower than is ideal, conditioning exercises are developed to help train the brain to run at what Tim Royer, the company’s founder, describes as “a sweet spot.”
According to Royer, Cousins’s data revealed that his brain was running faster than it should, relying on adrenaline much of the time. Readings of his cardiovascular system and respiratory system suggested a similar, over-stimulated condition that Royer likened to “somebody running from a lion.”
“When you try to play sports at an elite level and the body and brain are doing that, it makes it difficult over time,” Royer said in a telephone interview.
So he devised a training system to help Cousins regulate that speed and outfitted the quarterback with home-based gear to practice the exercises on his own.
In one such exercise, Cousins attaches the EEG leads to his scalp and connects it to a computer that displays the speed of his brain, heart and breathing as if it’s the dashboard of a car. Then comes the “reward system” that affirms when he has relaxed or conditioned his brain to operate in the sweet spot.
As Royer explains it, Cousins puts a movie in the computer, and a program driven by the electrical activity in the brain will play the movie only when the reading confirms that his brain is running in the optimum range.
In the early going, Royer said, Cousins might have been able to watch “Iron Man” for 20 seconds of a one-minute exercise. With practice, that period of time — time in which the brain is operated at an optimal speed — increased to 30 seconds, then 40.
On Sunday against Miami, Cousins will find himself staring at Iron Men of a different sort — lined up across from a Dolphins defensive line that Hall of Fame quarterback Dan Fouts believes is the best in the NFL.
“It’s a great opportunity for Cousins and an unbelievable challenge with that Dolphins front four,” said Fouts, who will provide commentary for the CBS broadcast. “He has to start fast and have success right away.”
Pro Bowl left tackle Trent Williams will protect Cousins’s blind side. But rookie Brandon Scherff and second-year player Morgan Moses must fend off the heart of Miami’s pass rush, sack-specialists Ndamukong Suh and Cameron Wake.
Cousins has the quickest release of the Redskins’ trio of quarterbacks, which should help. He also understands protections, Dolphins Coach Joe Philbin noted, able to bark out last-second adjustments. And he knows there’s no need for high-risk heroics after he makes a mistake, whether interception, fumble or sack.
Noting the gifted receiving and running back corps around him, Cousins said this week: “It’s my job to get them the football, then let them go do the jaw-dropping stuff.”
If boos rain down from a restive fan base, Cousins has heard them before. If he falls short of his own expectation, he has been there.
This year, if the offseason lessons stick, Cousins will take a deep breath. He will acknowledge to himself that, yes, it is a huge game, but he won’t let the magnitude paralyze him or send him into panic mode.
He will breathe deeply, settle his mind and call the next play.
Read the original article Here
- Comments (0)
- fMRI and EEG Study of Decision-Making Processes in Brain
- By Jason von Stietz, M.A.
- September 19, 2015
-
Photo Credit: Getty Images Researchers at the Institute for Neuroscience and Psychology at the University of Glasgow investigated the processes in the brain related to learning to avoid making mistakes and learning to make god decisions. The study simultaneously utilized EEG and fMRI allowing researchers to study decision-making in the brain with both the high temporal precision offered by EEG and the ability to detect precisely where these process are taking place in the brain offered by fMRI. The study was discussed in Neuroscience News:
Imagine picking wild berries in a forest when suddenly a swarm of bees flies out from behind a bush. In a split second, your motor system has already reacted to flee the swarm. This automatic response – acting before thinking – constitutes a powerful survival mechanism to avoid imminent danger.
In turn, a separate, more deliberate process of learning to avoid similar situations in the future will also occur, rendering future berry-picking attempts unappealing. This more deliberate, “thinking” process will assist in re-evaluating an outcome and adjusting how rewarding similar choices will be in the future.
“To date the biological validity and neural underpinnings of these separate value systems remain unclear,” said Dr Marios Philiastides, who led the work published in the journalNature Communications.
In order to understand the neuronal basis of these systems, Dr. Philiastides’ team devised a novel state-of-the-art brain imaging procedure.
Specifically, they hooked up volunteers to an EEG machine (to measure brain electrical activity) while they were concurrently being scanned in an MRI machine.
An EEG machine records brain activity with high temporal precision (“when” things are happening in the brain) while functional MRI provides information on the location of this activity (“where” things are happening in the brain). To date, “when” and “where” questions have largely been studied separately, using each technique in isolation.
Dr. Philiastides’ lab is among the pioneering groups that have successfully combined the two techniques to simultaneously provide answers to both questions.
The ability to use EEG, which detects tiny electrical signals on the scalp, in an MRI machine, which generates large electromagnetic interference, hinges largely on the team’s ability to remove the ‘noise’ produced by the scanner.
During these measurements participants were shown a series of pairs of symbols and asked to choose the one they believed was more profitable (the one which earned them more points).
They performed this task through trial and error by using the outcome of each choice as a learning signal to guide later decisions. Picking the correct symbol rewarded them with points and increased the sum of money paid to them for taking part in the study while the other symbol did not.
To make the learning process more challenging and to keep participants engaged with the task, there was a probability that on 30% of occasions even the correct symbol would incur a penalty.
The results showed two separate (in time and space) but interacting value systems associated with reward-guided learning in the human brain.
The data suggests that an early system responds preferentially to negative outcomes only in order to initiate a fast automatic alertness response. Only after this initial response, a slower system takes over to either promote avoidance or approach learning, following negative and positive outcomes, respectively.
Critically, when negative outcomes occur, the early system down-regulates the late system so that the brain can learn to avoid repeating the same mistake and to readjust how rewarding similar choices would “feel” in the future.
The presence of these separate value systems suggests that different neurotransmitter pathways might modulate each system and facilitate their interaction, said Elsa Fouragnan, the first author of the paper.
Dr Philiastides added: “Our research opens up new avenues for the investigation of the neural system underlying normal as well as maladaptive decision making in humans. Crucially, their findings have the potential to offer an improved understanding of how everyday responses to rewarding or stressful events can affect our capacity to make optimal decisions. In addition, the work can facilitate the study of how mental disorders associated with impairments in engaging with aversive outcomes (such as chronic stress, obsessive-compulsive disorder, post-traumatic disorder and depression), affect learning and strategic planning.
Read the original article Here
- Comments (0)
- Neuropsychoanalysis: An Emerging Field
- By Jason von Stietz
- September 12, 2015
-
Getty Images There is a new burgeoning field that combines two, often considered fundamentally different fields, neuroscience and psychoanalysis: neuropsychoanalysis. Although collaboration between these schools of thought seem surprising to many, it appeared obvious to Mark Solms, the pioneer of neuropsychoanalysis. This interesting new field was discussed in a recent article in The Atlantic:
I am in an apartment on the Upper East Side of Manhattan, surrounded by psychoanalysts. At moments, if I half close my eyes, I can imagine I’m in some European city, circa 1930: “The Kleinians have this very disturbing, I think, notion of countertransference as being something the patient does to you. They’re moving too far away from Freud’s understanding…” But in fact it’s 2010, and the conversation is new.
The experience of sitting on the edge of the huddle of analysts is, I imagine, like reading Dickens in the original serial: ongoing storylines, full of vivid characters, perpetually left in suspense. One analyst describes her work with Theo, a 30-year-old left in a wheelchair with global brain damage after a car accident, whose mother brought him to analysis with severe mental impairments and memory problems. Another discusses the progress he has made with Harry, left aphasic after a stroke, still able to comprehend but unable to express language.
Mark Solms, the neuropsychologist and psychoanalyst who founded this group in 2001, and continues to oversee its progress, is hardly the first to turn to brain damage seeking insight. Many of neuroscience’s greatest and most legendary discoveries have tumbled forth from damaged brains—from Phineas Gage, the 19th-century railroad worker whose frontal-lobe injury illuminated the brain mechanisms of self-control, to the patient known as H.M., whose radical surgery provided scientists with the ultimate test case for how the brain organizes memory.
But instead of waiting for these case studies to turn up, Solms decided to seek them out himself, and to see what might come from applying to their injuries an unorthodox means of investigation. Solms has spent his career bringing Freudian theory into the room where only biological fact had previously existed. He is a leading figure in a new interdisciplinary undertaking—along with a growing number of analysts, scientists, and others—named neuropsychoanalysis.
In the popular imagination, the term “psychoanalysis” conjures up silent doctors in dimly lit rooms, witnesses to the unfurling of dream images and childhood memories. And couches, lots of couches. This is the stereotype, the myth, but the field wielded an enormous authority throughout the 20th century, and continues to influence our most basic assumptions about human nature, like the power of the unconscious mind, the profound importance of early childhood experience, and the fact that memory is fundamentally dynamic.
Psychoanalysis has since taken on the aspect of the underdog. Many—maybe most—are unwilling to call the study of inner reality, psychic conflicts, dynamic forces and repressed material a science. And until recently, there has been relatively little empirical proof that psychoanalysis even works. Up against the quick and easy fixes of prescription medication or short-term, practically oriented cognitive-behavioral therapy—and under the skeptical eye of insurance companies—psychoanalysis faces an uncertain future.
Today, neuroscience is the golden child, commanding newspaper headlines, substantial government grants, and an ever-increasing portion of the public imagination. With its armament of modern tools and acronyms, it offers a seemingly endless list of options for looking at the brain. Neuroscientific findings are morphing into cultural truths: We are “hardwired,” a collection of parts, of “circuits” and “networks” that “light up” when “activated.” The brain has become our modern metaphor; it is where we look to find out what’s really going on. Already, neuroscientific research has penetrated the field of economics, the courts, and beyond. It is decidedly less common to hear psychoanalytic concepts invoked in these same circles.
With their starkly different goals, methods, and cultures, psychoanalysis and neuroscience can appear to be two different species, mutually alienated, as if preoccupied with two altogether different pursuits. But to some, like Solms, they are merely two views of the same object. Psychoanalysis looks at the brain from the inside out: What does it feel like to be this thing? Neuroscience looks at the brain from the outside in, measuring its behavior, investigating its physical mechanisms.
Solms supervises the progress of his group of New York psychoanalysts on monthly trips from South Africa. Tall, solid, and thick-wristed, Solms is in his late forties, but looks older. His gray hair, poking up in all directions, is completely unattended to, like a member of the family with whom he is no longer on speaking terms. In New York, he listens to developments in the group’s roster of psychoanalytic cases. In Cape Town, he is a professor of neuropsychology, making rounds in the University of Cape Town’s teaching hospital, and chairing the university’s neuropsychology department. He leads a kind of double life—one that began in the early days of his career, when he worked with brain-damaged patients by day at the Royal London Hospital, training at the Institute of Psychoanalysis by night.
Solms first trained in neuropsychology—a branch of neurology that draws links between people’s external behaviors and the specific regions of the brain involved in producing them—thinking that of all the subsets of neuroscience, neuropsychology was, as he puts it, “where you’re most likely to find out about the person himself.” But he was disappointed. Neuropsychology seemed to avoid everything that had to do with questions of personality, emotion, motivation—in other words, the things we mean when we speak of “human nature.” Instead, the operating gaze was trained onto the strictly quantifiable: How many digits could the patient hold in his working memory? Neuropsychology, Solms discovered, asked black-and-white questions that could be answered on standardized tests.
“Oliver Sacks has this saying: Neuropsychology is admirable, but it excludes the psyche,” Solms says.
Solms first heard of Freud as an undergraduate, when he stumbled across a seminar in the comparative literature department. He showed up a few weeks after the start of the semester, just as the class was assigned Freud’s lesser-knownProject for a Scientific Psychology, a summary of his attempts grapple with neurology in the years before he turned his full attention to the psychological. After completing his training as a neuropsychologist, Solms began to school himself in Freud’s ideas in earnest, and when he moved to London in his late twenties, began to train as a psychoanalyst. For the past decade, in his off hours, he has been working on the revision of James Strachey’s original English translation of the complete Standard Edition of Freud, all twenty four volumes. He often wonders what he’s gotten himself into.
It took Solms some time to understand that his inclination to combine two branches of psychology would be seen by many as controversial or problematic; that the two disciplines, psychoanalysis and neuroscience, are mostly indifferent to each other, and even, at times, opposed. But for Solms, they were intuitively compatible.
“I say it was obvious to me—why wasn’t it obvious to everyone?” Solms told me. “Like everything else, it was personal. My brother was brain-injured. When he was 6, he fell off the roof and suffered a closed head injury. I saw that my brother is not who he was. His personality is different and our whole family is different. All of that because this organ is not functioning as it was before.”
Solms and his work have a magnetic pull. People uproot their lives and come to South Africa to enter into his orbit. When I visited Solms in Cape Town, there were two such examples on hand: a Swiss expert on neuropeptides and a psychoanalyst from Vienna, both of whom had both moved to Cape Town specifically to work with Solms. The latter was preparing to begin a study that Solms had designed: psychoanalyzing a population of patients with Urbach-Wiethe disease, an extremely rare genetic disorder in which a person’s amygdala gradually calcifies until it is almost completely defunct. Solms was particularly interested in what effect this might have on the content of their dreams.
“Biology is truly a land of unlimited possibilities. We may expect it to give us the most surprising information, and we cannot guess what answers it will return in a few dozen years to the questions we have put to it.”
So reflected Freud in 1920. Having spent 20 years toiling away in labs, peering down microscopes, he arrived at the conclusion that the questions he wanted to answer about the human mind couldn’t be answered by what was then understood—or understandable—about the human brain. The knowledge wasn’t there, and neither were the tools. He continued to emphasize, however, that eventually, long after his own lifetime, the moment would come when brain science would be ready to fill out the psychoanalytic principles that he was busy laying down. Solms and his followers believe that moment is here.
It can be difficult to see how someone like Solms fit into the neuroscientific landscape. To say “Freud” to scientists engaged in the pursuit of empirical truths is to risk making yourself instantly suspect and quickly irrelevant. Yet however unlikely the idea, however unimaginable the design, neuropsychoanalysis may offer something valuable: a sketch of inner life where creativity isn’t simply explained as patterns of electrical waves, sadness as the number you circle between one and nine, and love confused with the mating habits of prairie voles.
As Solms told me: “There can’t be a mind for neuroscience and a mind for psychoanalysis. There’s only one human mind.”
Read the original article Here
- Comments (0)
- The Neural Activity of Happy Older Couples
- By Jason von Stietz
- September 4, 2015
-

Photo Credit: Getty Images Does being in a long-term and committed relationship change our neural activity? Researchers at the Rotman Research Institute Toronto and University of Toronto studied the brain scans of 14 older adult women while they viewed of either their husbands or strangers. One interesting finding was that women who reported higher relationship satisfaction showed greater activation in brain regions containing mirror neurons. The study was discussed in a recent article in Slate:
Have you ever waited with excitement to share some amazingly good news with your partner, only to experience a surge of frustration and resentment when he or she barely reacts to your announcement? As a society, we place a huge amount of emphasis on being there for each other when we’re in need, but past research has actually shown that relationship satisfaction is influenced as much, if not more, by how we react to each other’s good news. Whereas emotional support from a partner when we’re down can have the unfortunate side-effect of making us feel indebted and more aware of our negative emotions, a partner’s positive reaction to our good news can magnify the benefits of that good fortune and make us feel closer to them.
Now an unusual brain-imaging study, published recently in Human Brain Mapping, has added to this picture, showing that the relationship satisfaction of longtime married elderly women is particularly related to the neural activity they show in response to their husbands’ displays of positive emotion, rather than negative emotion.
Psychologist Raluca Petrican at the Rotman Research Institute in Toronto and her colleagues at the University of Toronto recruited 14 women with an average age of 72 who’d been married for an average of 40 years. The researchers scanned these women’s brains as they watched some carefully prepared videos.
The silent ten-second videos showed each woman’s husband or a stranger displaying an emotion that mismatched the way the video clip was labeled in a one-sentence description on the screen. For example, the clip might show the husband smiling or laughing about a happy memory (such as the first house they bought), but the video was labeled misleadingly to suggest that the man was showing this emotion while talking about a sad memory (such as the time he got fired). Other videos showed the reverse mismatch: a negative emotional display, ostensibly shown while talking about the memory of a happy event.
Essentially, the videos were designed to make the women feel like they were seeing their husband or the stranger display a surprising emotional reaction that didn’t match their own feelings. The real-world equivalent would be a situation in which a husband is happy about something that his wife doesn’t “get”; and the questions are whether she will notice, and whether she is she more sensitive to this incongruent emotion in her husband than she would be in a stranger.
The first important finding to emerge from this setup was that the women showed enhanced overall brain activity—which suggests more mental and emotional neural processing —when watching the videos of their husbands compared with videos of the strangers, but only when the videos showed displays of surprisingly incongruent positive emotion. During the other types of videos (when the men appeared to display strangely negative emotion), the women’s brains showed just as much overall activity when watching a stranger as when watching their husband. In other words, their levels of whole-brain activity betrayed a special sensitivity to their husband’s (versus a stranger’s) unexpected positive emotion.
This jibes with the past research that’s shown it’s our response to our partners’ positive news that is all-important for relationship satisfaction. Remember that these women had been married for decades, so it’s likely that they and their husbands have been doing something right relationship-wise. The brain-imaging data suggest part of the reason might be that the women are acutely tuned to when their husbands are showing happiness that’s personal to them (rather than common to both partners).
This specific interpretation trips up a little with another main result: The women’s levels of marital satisfaction (according to a questionnaire) correlated with the amount of neural processing they showed in response to their husbands’ positive and negative emotion.
However, the special importance of how we respond to our partners’ positive emotion was supported by another key finding. Namely, women who scored higher on relationship satisfaction showed more brain activation in regions thought to contain mirror neurons (neurons that are considered important for empathy) when watching their spouses than they did when watching a stranger. Moreover, this enhanced mirror-neuron activity was especially present for the videos showing their husbands’ positive, rather than negative, emotion. Again, this appears to support the idea that marital happiness goes hand in hand with sensitivity to our partners’ positive emotion (though the researchers acknowledge a different or complementary interpretation that people in happy relationships have a suppressed response to their partners’ incongruent negative emotion).
We need to interpret these preliminary and complex findings with caution. And the exclusive focus on wives’ reactions to their husbands’ emotions does lend the study a slightly retro ’70s vibe—what about the way that husbands respond to their wives’ emotions, and the importance of that for the marital happiness of both parties? But that said, the results are tantalizing in suggesting that at a neural level, people in a long-term, committed relationship are especially sensitive to their partners’ positive emotion, and particularly so when this emotion is different from their own. This neatly complements other past research showing, for example, that people who are unable to differentiate their partners’ emotions from their own (they assume they’re the same), tend to be viewed by their partners as more controlling and smothering.
As a whole, this entire body of research gives pause for thought. How do you react when your partner arrives home on an emotional high? Would you only notice if you were feeling happy too?
Read the original article Here
- Comments (0)
- Neuroscience of Indecision
- By Jason von Stietz
- August 24, 2015
-
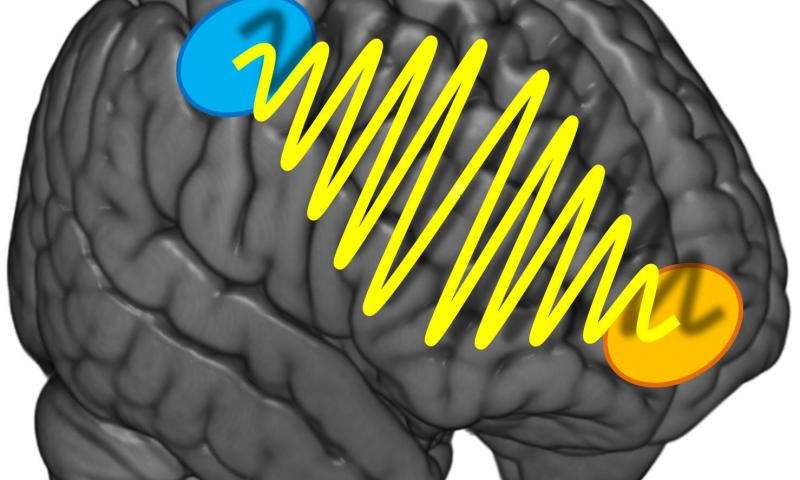
Photo Credit: University of Zurich Why is it sometimes so hard to decide what we are in the mood to eat for dinner? Should we order the steak or the veal? Researchers at the University of Zurich found that indecisiveness relates to the strength of communication between two different regions of the brain. The study was discussed in a recent article in Medical Xpress:
It's the same old story: You're in a restaurant and can't make up your mind what to order. After studying the menu for some time and many discussions, you eventually choose the steak. But you can't relax during the meal and keep wondering whether you should have gone for the veal after all. Such difficulties with decisions crop up in all aspects of life, not only food. However, they predominantly affect preference-based decisions, i.e. questions like «what do I prefer - melon or cherries?" Purely sensory decisions based on sensorial information such as «what is bigger - melon or cherry?" are less prone to indecisiveness.
The more intensive the information flow, the more decisive
How come some people are so uncertain of their preferences and keep making new choices while others know exactly what they like and want? A team headed by Professor Christian Ruff, a neuroeconomist from the University of Zurich, set about investigating this question. The Zurich researchers discovered that the precision and stability of preference decisions do not only depend on the strength of the activation of one or more brain regions. Instead, the key for stable preference choices is the intensity of the communication between two areas of the brain which represent our preferences or are involved in spatial orientation and action planning.
The researchers used transcranial alternating current stimulation, a non-invasive brain stimulation method that enables generation of coordinated oscillations in the activity of particular brain regions. The test subjects did not realize that they were being stimulated. Using this technique, the researchers intensified or reduced the information flow between the prefrontal cortex located directly below the forehead and the parietal cortex just above both ears. The test subjects had to make preference-based or purely sensory decisions about food.
«We discovered that preference-based decisions were less stable if the information flow between the two brain regions was disrupted. Our test subjects were therefore more indecisive. For the purely sensory decisions, however, there was no such effect," explains Ruff. «Consequently, thecommunication between the two brain regions is only relevant if we have to decide whether we like something and not when we make decisions based on objective facts." There was no evidence of any gender-specific effects in the experiments.
It was not possible to make the decisions more stable by intensifying the information flow. However, the study participants were young, healthy test subjects with highly developed decision-making skills. On the other hand, the results of the study could be used for therapeutic measures in the future - such as in patients who suffer from a high degree of impulsiveness and indecisiveness in the aftermath of brain disorders.
Read the original article Here
- Comments (0)
- Brain Scans Predict Success of CBT for Social Anxiety Disorder
- By Jason von Stietz
- August 20, 2015
-
.jpg)
Photo Credit: MIT News Social anxiety disorder (SAD) affects 15 million people in the United States, approximately 6.8 percent of the U.S. population. Unfortunately, many treatments of SAD succeed as often as they fail. However, researchers at MIT found that brain scans predicted which patients would benefit from CBT with an accuracy of 80 percent. Medical Xpress discussed the findings in a recent article:
For patients with social anxiety disorder (SAD), current behavioral and pharmaceutical treatments work about half the time. After weeks of investment in therapy, about half of patients will likely still suffer with symptoms of anxiety, and have little choice but to try again with something else. This trial-and-error process—inevitable due to an absence of tools to guide treatment selection—is time-consuming and expensive, and some patients eventually just give up.
But new MIT research suggests that it may be possible to do better than a coin toss when choosing psychiatric therapies for patients. The study, which performed brain scans on 38 SAD patients, found that these scans contain clues that indicate, with about 80 percent accuracy, which SAD patients will do well in cognitive behavioral therapy (CBT), an intervention designed to help patients change thinking patterns. Use of the scans to predict treatment outcomes improved predictions fivefold over use of a clinician's assessment alone.
"Choice of therapy is like a wheel of chance," says first author Susan Whitfield-Gabrieli, a research scientist in the McGovern Institute for Brain Research at MIT. "We're hoping to use brain imaging to help provide more reliable predictors of treatment response."
The researchers used a form of brain imaging that scans patients in a state of rest. Resting-state images can be done quickly, in about 15 minutes, and reliably, since they don't require patients to follow instructions, so they have the potential to be used in a clinical setting as a tool that helps doctors select the best treatments for patients.
"Knowing who to give which therapy to upfront would save time, money, and health care resources," says Greg Siegle, an associate professor of psychiatry at the University of Pittsburgh School of Medicine who was not involved in this study. "This ability would be staggering to have at our disposal for the health care system."
The findings are reported in the current issue of the journal Molecular Psychiatry. The work was carried out in the lab of principal investigator John Gabrieli, the Grover Hermann Professor of Health Sciences and Cognitive Neuroscience at MIT and a member of the McGovern Institute.
Common disorder
Social anxiety disorder affects approximately 6.8 percent of Americans, about 15 million individuals, and is the country's third-most-common mental health disorder, according to the National Institutes of Mental Health. Its symptoms include extreme anxiety in social settings that can interfere with work and quality of life. Patients living with this disorder are also at higher risk of other psychiatric disorders, such as depression and substance abuse.
The study analyzed SAD patients from the Center for Anxiety and Related Disorders at Boston University and the Center for Anxiety and Traumatic Stress at Massachusetts General Hospital. The patients were scanned prior to participation in 12 weeks of group-based CBT. They also were evaluated using a behavioral assessment tool called the Liebowitz Social Anxiety Scale (LSAS) before and after CBT to determine who had improved.
In 2013, co-author Satrajit Ghosh, a principal research scientist at the McGovern Institute, studied task-based scans of this same group of patients. He and Whitfield-Gabrieli found that scans of patients' brains as they responded to angry or neutral faces and emotional or neutral scenes predicted CBT outcomes.
"But task-based scans have downsides," Whitfield-Gabrieli says: Behavioral differences among patients can affect performance. Also, task-based scans can only be used on patients who can follow a task, which excludes infants and some elderly or very ill patients.
Scanning the resting brain
So Whitfield-Gabrieli followed this earlier research with a study of the predictive power of resting-state imaging, which she and colleagues had also performed prior to CBT. During a resting-state scan, the patient just lies there. "That's the beauty of it," she says. "They're just letting their minds wander."
Resting-state imaging provides a look at the way a patient's brain is wired, both structurally and functionally. For instance, resting-state functional magnetic resonance imaging (fMRI) shows which parts of the brain synchronize with one another during rest, suggesting that they are functionally connected. In addition, analysis of diffusion-weighted magnetic resonance imaging (dMRI) shows the underlying anatomy of the white matter tracts that interconnect distant brain regions.
Based on findings from their earlier research, Whitfield-Gabrieli and colleagues first used resting-state fMRI to look at connections to the amygdala, the seat of fear in the brain. They found that patients with higher connectivity to the amygdala from certain other regions were more likely to have lower anxiety after CBT.
They then performed a second analysis of the resting-state fMRI data, this time looking across the entire brain for patterns of connectivity. This analysis revealed additional markers that were predictive of treatment. The researchers also analyzed dMRI data and found that more robust connectivity in the tract that connects visual cues with emotional responses is also predictive of improvement with CBT.
Higher LSAS scores, which indicate more severe SAD, correlate modestly with larger improvements after CBT. In this study, each brain scan analysis had predictive value beyond the LSAS, and the three analyses together produced a fivefold improvement in predictive power over the LSAS alone.
The next step for Whitfield-Gabrieli and colleagues is to validate their predictive model on hundreds or possibly thousands of patients. Such a large-scale study may be possible because resting-state scans are comparable even when performed in different labs or by different researchers. Such comparisons weren't feasible using task-based scans, which tend to vary from lab to lab.
"Right now there's a huge movement to create massive data sets, to share resting-state imaging data, and really change the way people do science," Whitfield-Gabrieli says.
Other next steps for Whitfield-Gabrieli's group are studies to predict the success of more than one form of therapy, and to look at other psychiatric conditions, such as depression and attention disorders. "We don't want to just know if they're going to respond to one treatment," she says. "We want to know which treatment is best for each patient."
Read the original article Here
- Comments (0)
- Electrical Signals Might Facilitate the Repair of Spinal Cord Injuries
- By Jason von Stietz
- August 7, 2015
-

Researcher Li Yao. Photo Credit: Wichita State University Can the spinal cord heal itself after an injury? A researcher at Wichita State University is investigating a promising new approach that involves aiming electrical signals at the spinal cord that facilitate healing. A recent article in NeuroScientistNews discusses the new approach:
Wichita State University's Li Yao is taking a special approach to the study of spinal cord injuries through research that uses an electrical signal to repair tissue damage.
When a person suffers neurological damage to their spinal cord, the tissues surrounding the injury site can die. But one of the body's defense mechanisms is the regeneration and migration of a type of support cell -- called Schwann cells -- to the injury.
Those cells, as has been discovered in recent years, help myelinate -- or cover -- nerve axons where the injury has occurred, which promotes the recovery of some of the spinal cord's function.
Yao, a biological sciences assistant professor, is studying how electrical signals can aim those cells directly to the injury site. His research, he hopes, will open new doors for the medical field to use electrical fields in the treatment of neural injuries.
"Electrical signal is a kind of ignored approach that may generate significant biological function in neural regeneration," Yao says.
Yao's research studies the molecular mechanism of cell migration in electric fields using next-generation RNA sequencing to look at the signaling pathways that regulate cell migration.
So far, he has discovered that the precision of the cell migration toward the injury increased significantly as the strength of the electrical field increased. The electrical field did not, however, change the speed at which the cells moved.
Still, Yao's early findings suggest that the use of electrical fields in cell migration could become a burgeoning area of study in regenerative medicine.
"Our work has implications for central nervous system repair, and the application of an electrical field may assist with that," Yao says.
Read the original article Here
- Comments (0)
- Transcranial Magnetic Stimulation: A Non-Drug Treatment Option for Depression
- By Jason von Stietz
- July 29, 2015
-
Photo Credit: Getty Images It is estimated that 7 percent of people in the United States live with clinical depression. Transcranial magnetic stimulation (TMS), involves stimulating the prefrontal cortex, which is found to be under-activated in people with depression. TMS is a non-drug treatment option that is beginning to find favor among clinicians and researchers, alike. A recent article in the Tribune discussed the empirical research and the experience of clinicians supporting TMS:
Depression lifted from Nick O'Madden's life like a set of foggy glasses being wiped clean.
Earlier this summer, O'Madden, 31, felt he was living in a distracted haze, sprinkled with nighttime panic attacks. Now, after undergoing an emerging high-tech treatment involving magnetic currents, he said he's literally seeing the world in a new light.
"Colors are brighter," said O'Madden, a mental health therapist who lives in Elk Grove, Calif. "Last night, I was looking at the moon, and it just looked clearer and brighter and more beautiful ... It's almost kind of scary to see that at first, it's so new to me."
He described the changes from a reclined medical chair at TMS Health Solutions, a treatment center in Sacramento's Campus Commons area that specializes in transcranial magnetic stimulation. With a metal coil positioned near his forehead, he spoke between bouts of jackhammer-esque pulsing that erupted every 15 seconds during the 50-minute session.
The "train pulses," as technicians call the strings of sound, are actually the back-and-forth flexing of the metal coil as the device sends out a 2-tesla-strong magnetic current. The coil creates a magnetic field that reaches 2 to 3 centimeters into brain matter to stimulate the dorsal-lateral prefrontal cortex, the poker chip-sized area responsible for regulating mood, memory and decision-making.
An estimated 7 percent of American adults suffer from clinical depression, which can cause lethargy, indifference, moodiness and other symptoms that interfere with day-to-day functioning. Researchers have found that the prefrontal cortex is often underactive in people diagnosed with the illness.
The TMS technology uses electric currents to excite cell activity in that part of the brain, theoretically helping neurons better communicate with one another and increasing blood flow to the tissue, which promotes healthy brain function. The federal Food and Drug Administration has approved the treatment, but for limited use given that it is relatively new. Physicians can administer it only to patients who haven't responded to at least one prescription medication for depression.
Advocates of the treatment refer to it as revolutionary; there hasn't been a major development in procedure-based depression treatment since the advent of electroconvulsive therapy. Unlike that treatment, which applies electricity directly to the skull to invoke a brain seizure, the magnetic TMS procedure has not shown negative impact on memory or cognition.
TMS, and other new treatments that focus on physical stimulation of specific parts of the brain, signal a departure from traditional methods of treating mental illness, such as talk therapy and prescription drugs. As advances in medical technology allow researchers to better understand how the human brain functions, approaches to treatment are following suit.
"There's a growing recognition, both with scientists and patients, that depression is a brain problem - a problem with chemicals in our circuitry," said Dr. Paul Croarkin, a psychiatrist with the Mayo Clinic. "The fact that we're soon going to have more and more offerings in that regard is a positive thing."
As with many emerging medical treatments, practitioners and insurers hesitate to embrace new procedures without a solid track record. Though the FDA approved the nation's first TMS device in 2008, major health insurance companies have only begun covering the treatment in the past few years.
Dr. Richard Bermudes is principal owner and medical director of TMS Health Solutions and president of the nationwide Clinical TMS Society. By his estimate, about 700 TMS devices are in use in the United States.
The treatment has been the focus of about 30 randomized clinical trials in the United States, and in most of those, a statistically significant portion of patients were determined to have benefited. But some researchers caution that the improvements could be the result of a placebo effect, and have called for longer-term studies.
A 2012 study published in the Journal of Clinical Psychiatry showed that half of the patients involved in that trial responded to the treatment within six weeks, and 25 percent went into remission. Still, guidelines from the Agency for Healthcare Research and Quality and the Department of Health and Human Services state that evidence is "insufficient to evaluate the ability of (repetitive) TMS to maintain response or remission."
On the upside, the therapy has not been shown to cause whole-body side effects, such as weight gain or fatigue, as an oral medication might, said Dr. Guohua Xia, a clinical associate professor at University of California-Davis and medical director of Brainefit, a mental health institute offering a form of TMS services. That means it can be especially helpful for pregnant women and elderly people who may experience problems with standard depression drugs.
Sutter Health is the only hospital system in Sacramento to offer the treatment. Dr. Theodore Goodman, director of interventional psychiatry for Sutter Health, said TMS has resulted in improvement for about 60 percent of patients during the two years it has been offered at the Sutter Center for Psychiatry.
He expressed frustration at insurance companies not covering the treatment long term. TMS is currently approved only as a treatment for acute clinical depression, meaning patients are in the throes of symptoms.
"About 50 percent of patients will relapse over a year's time," he said. "The way you avoid that is maintenance treatment, but insurance won't pay for that. It's a horribly unenlightened viewpoint."
While NeuroStar, the model used at Bermudes' clinic, was the first TMS device approved on the market, other brands go even further into brain matter and have been used to target other conditions, including migraines.
At TMS Health Solutions, the recommended treatment plan is four to six weeks of daily TMS sessions, at a cost of $5,000 to $7,000. Since opening clinics in El Dorado Hills, Calif., in 2007 and Sacramento in 2010, Bermudes said, he has used the technology to treat hundreds of patients and currently sees about 20 TMS patients a day.
He said he recently changed the clinic's name - from Mindful Health Solutions - specifically to highlight the treatment.
"There's not a lot of access to this modality currently in the community," he said. "A lot of our patients have been depressed for years before coming to TMS. If we can get people into TMS earlier, our remission and response rates may go up."
O'Madden said that, for him, improvement came after three weeks of treatment, though technicians say results can take longer. Before his physician suggested TMS, O'Madden said, he was having trouble sleeping and focusing, and struggled to control anxiety and obsessive thought patterns.
He said he's now feeling more focused and active, with a renewed passion for boxing. He recently started a blog to document his recovery.
"I want people to become more aware of (TMS), and I also want mental health to be less stigmatized," he said. "I want people to see me as a person: I'm a father and a husband, but I suffer from a mental health disorder, and I'm seeking help ... and other people can do the same thing."
Read the original article Here. For additional information about TMS visit Brain Wellness Center. Brain Wellness Center is located in San Ramon and Palo Alto and is one of the leading edge providers of TMS services. Each patient’s qEEG brain mapping information is utilized to customize and tailor make the treatment to their specific and unique brain pattern.
- Comments (8)


 Subscribe to our Feed via RSS
Subscribe to our Feed via RSS